Heart Conditions — Arrhythmia
Atrial
Fibrillation
Atrial fibrillation is the most common sustained heart rhythm disorder, affecting around 10% of people over 70. It carries a significant stroke risk and is eminently treatable — but it must first be identified and properly assessed.
The Most Common Arrhythmia
What Is Atrial Fibrillation?
In a normal heart, a regular electrical signal from the sino-atrial node coordinates each heartbeat. In atrial fibrillation, the upper chambers (atria) fire chaotically — hundreds of times per minute — producing a rapid, completely irregular rhythm in the lower chambers (ventricles).
AF becomes increasingly prevalent with age, affecting approximately 10% of people over 70. The primary risk factors are advancing age, hypertension, alcohol use, thyroid disorders, obesity, and sleep apnoea.
Patients typically describe sensations of uncontrolled heart activity — fluttering, racing, or an irregular thumping. Some patients, however, have no symptoms at all, and AF is discovered only on a routine ECG or when a stroke occurs — making proactive screening important in those with risk factors.
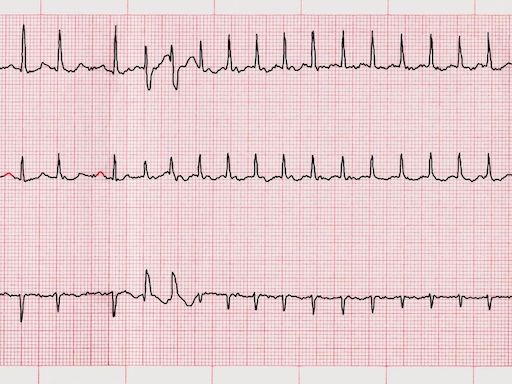
Classification
The Three Types of AF
AF is classified by how it behaves over time. Understanding the type helps determine both the urgency of treatment and the likelihood of restoring a normal rhythm.
Paroxysmal AF
Episodes that start and stop on their own
Episodes terminate spontaneously, usually within 48 hours but by definition within 7 days. Patients may have frequent episodes or very infrequent ones. Paroxysmal AF still carries a stroke risk and warrants anticoagulation assessment. Rhythm-control strategies to reduce burden are most effective early in the disease course.
Persistent AF
Continuous AF lasting more than 7 days
AF does not self-terminate and requires medical intervention — either cardioversion (electrical reset of the heart) or medication — to restore normal rhythm. The longer AF is present, the more the atria remodel, making rhythm restoration progressively less successful.
Permanent AF
When restoring normal rhythm is no longer possible or pursued
The decision to accept permanent AF focuses management on controlling the heart rate, preventing stroke with anticoagulation, and managing symptoms. Anticoagulation remains essential throughout.
The Most Serious Complication
AF & Stroke Risk
During atrial fibrillation, the atria lose their coordinated contraction. Blood pools and stagnates in the left atrial appendage — a small pouch off the upper chamber — allowing clots to form. These clots can then travel to the brain, causing a potentially devastating and often permanent stroke.
AF-related strokes tend to be severe, as large clots can block major cerebral arteries. The CHA₂DS₂-VASc scoring system quantifies stroke risk by accounting for the patient's age, sex, and other cardiovascular conditions. Patients scoring 2 or above are typically recommended anticoagulation therapy.
Modern DOACs (Direct Oral Anticoagulants) such as apixaban, rivaroxaban, and edoxaban have largely replaced warfarin. They are highly effective, require no regular blood monitoring, and have a better safety profile for most patients.
CHA₂DS₂-VASc Score Factors
- CCongestive heart failure1 pt
- HHypertension1 pt
- A₂Age 75 or over2 pts
- DDiabetes mellitus1 pt
- S₂Prior stroke or TIA2 pts
- VVascular disease (heart attack, PAD)1 pt
- AAge 65–741 pt
- ScSex category (female)1 pt
Score of 2 or above in men (3 or above in women) — anticoagulation is recommended. Dr Nijjer will calculate your score and explain what it means for you.
Investigation
Tests for Atrial Fibrillation
AF may be present on a standard ECG, or it may be paroxysmal and require prolonged monitoring to capture. Structural assessment of the heart is always necessary.
- ECGAn irregular rhythm with absent P-waves confirms AF when present during the recording. If AF is paroxysmal, the resting ECG may be normal.
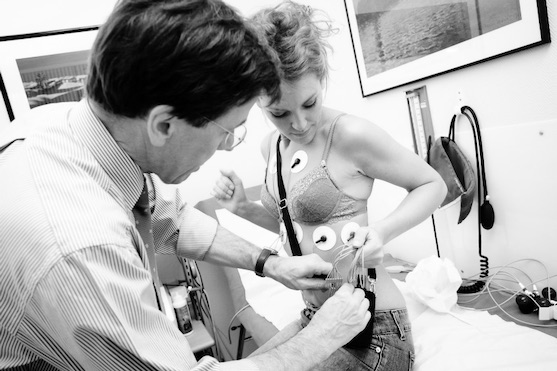
- Holter Monitor24–48 hour or longer ambulatory ECG monitoring to capture paroxysmal episodes and quantify AF burden over time.
- EchocardiogramAssesses heart structure, valve function, atrial size, and pumping function — all relevant to both cause and treatment planning.
- Blood TestsThyroid function (hyperthyroidism drives AF), kidney function (affects anticoagulant dosing), electrolytes, and full blood count.
- ElectrophysiologyFor selected patients being considered for ablation, detailed mapping of the heart's electrical system guides the procedure.
Management Options
Treating Atrial Fibrillation
AF management has three pillars: preventing stroke, controlling symptoms by managing rate or rhythm, and addressing any underlying causes. Dr Nijjer tailors the strategy to each patient's type of AF, symptoms, and overall health.
Anticoagulation
The single most important intervention for most AF patients. DOACs (apixaban, rivaroxaban, edoxaban) are preferred over warfarin for most patients due to their reliability, safety, and freedom from frequent blood tests.
Rate-Controlling Medications
When AF is accepted, controlling the resting and exercise heart rate to comfortable levels reduces symptoms and protects the heart muscle from rate-related weakening.
- Beta-blockers (bisoprolol, carvedilol)
- Rate-limiting calcium channel blockers
- Digoxin (in selected patients)
DC Cardioversion
A brief controlled electrical shock under sedation resets the heart to normal rhythm. Most effective when performed early. Anticoagulation is required for several weeks before and after the procedure.
AF Ablation
A catheter procedure targeting the electrical triggers of AF — typically around the pulmonary veins in the left atrium. Targeted burns (radiofrequency) or freezing (cryo-ablation) isolate the triggers. Most effective for paroxysmal AF in younger, earlier-disease patients.
Related Conditions
Further Reading
Palpitations
AF is the most common cause of sustained palpitations. Understanding what palpitations are and what investigation is needed helps put AF in the wider picture.
Learn about Palpitations → Risk FactorHigh Blood Pressure
Hypertension is the most common cause of AF. Treating blood pressure effectively can prevent AF from developing or reduce its burden once present.
Learn about Hypertension → ProcedurePacemakers
Some patients with AF develop dangerously slow heart rates requiring pacemaker implantation to maintain an adequate heart rate while rate-controlling medications are used.
Learn about Pacemakers →Diagnosed with atrial fibrillation?
Dr Nijjer offers expert AF assessment and management at 68 Harley Street — including stroke risk assessment, rate and rhythm control planning, cardioversion, and referral for ablation where appropriate.
Heart Conditions — Arrhythmia
Atrial
Fibrillation
Atrial fibrillation is the most common sustained heart rhythm disorder, affecting around 10% of people over 70. It carries a significant stroke risk and is eminently treatable — but it must first be identified and properly assessed.

The Most Common Arrhythmia
What Is Atrial Fibrillation?
In a normal heart, a regular electrical signal from the sino-atrial node coordinates each heartbeat. In atrial fibrillation, the upper chambers (atria) fire chaotically — hundreds of times per minute — producing a rapid, completely irregular rhythm in the lower chambers (ventricles).
AF becomes increasingly prevalent with age, affecting approximately 10% of people over 70. The primary risk factors are advancing age, hypertension, alcohol use, thyroid disorders, obesity, and sleep apnoea.
Patients typically describe sensations of uncontrolled heart activity — fluttering, racing, or an irregular thumping. Some patients, however, have no symptoms at all, and AF is discovered only on a routine ECG or when a stroke occurs — making proactive screening important in those with risk factors.

Classification
The Three Types of AF
AF is classified by how it behaves over time. Understanding the type helps determine both the urgency of treatment and the likelihood of restoring a normal rhythm.
Paroxysmal AF
Episodes that start and stop on their own
Episodes terminate spontaneously, usually within 48 hours but by definition within 7 days. Patients may have frequent episodes or very infrequent ones. Paroxysmal AF still carries a stroke risk and warrants anticoagulation assessment. Rhythm-control strategies to reduce burden are most effective early in the disease course.
Persistent AF
Continuous AF lasting more than 7 days
AF does not self-terminate and requires medical intervention — either cardioversion (electrical reset of the heart) or medication — to restore normal rhythm. The longer AF is present, the more the atria remodel, making rhythm restoration progressively less successful.
Permanent AF
When restoring normal rhythm is no longer possible or pursued
The decision to accept permanent AF focuses management on controlling the heart rate, preventing stroke with anticoagulation, and managing symptoms. Anticoagulation remains essential throughout.
The Most Serious Complication
AF & Stroke Risk
During atrial fibrillation, the atria lose their coordinated contraction. Blood pools and stagnates in the left atrial appendage — a small pouch off the upper chamber — allowing clots to form. These clots can then travel to the brain, causing a potentially devastating and often permanent stroke.
AF-related strokes tend to be severe, as large clots can block major cerebral arteries. The CHA₂DS₂-VASc scoring system quantifies stroke risk by accounting for the patient's age, sex, and other cardiovascular conditions. Patients scoring 2 or above are typically recommended anticoagulation therapy.
Modern DOACs (Direct Oral Anticoagulants) such as apixaban, rivaroxaban, and edoxaban have largely replaced warfarin. They are highly effective, require no regular blood monitoring, and have a better safety profile for most patients.
CHA₂DS₂-VASc Score Factors
- CCongestive heart failure1 pt
- HHypertension1 pt
- A₂Age 75 or over2 pts
- DDiabetes mellitus1 pt
- S₂Prior stroke or TIA2 pts
- VVascular disease (heart attack, PAD)1 pt
- AAge 65–741 pt
- ScSex category (female)1 pt
Score of 2 or above in men (3 or above in women) — anticoagulation is recommended. Dr Nijjer will calculate your score and explain what it means for you.
Investigation
Tests for Atrial Fibrillation
AF may be present on a standard ECG, or it may be paroxysmal and require prolonged monitoring to capture. Structural assessment of the heart is always necessary.
- ECGAn irregular rhythm with absent P-waves confirms AF when present during the recording. If AF is paroxysmal, the resting ECG may be normal.
- Holter Monitor24–48 hour or longer ambulatory ECG monitoring to capture paroxysmal episodes and quantify AF burden over time.
- EchocardiogramAssesses heart structure, valve function, atrial size, and pumping function — all relevant to both cause and treatment planning.
- Blood TestsThyroid function (hyperthyroidism drives AF), kidney function (affects anticoagulant dosing), electrolytes, and full blood count.
- ElectrophysiologyFor selected patients being considered for ablation, detailed mapping of the heart's electrical system guides the procedure.

Management Options
Treating Atrial Fibrillation
AF management has three pillars: preventing stroke, controlling symptoms by managing rate or rhythm, and addressing any underlying causes. Dr Nijjer tailors the strategy to each patient's type of AF, symptoms, and overall health.
Anticoagulation
The single most important intervention for most AF patients. DOACs (apixaban, rivaroxaban, edoxaban) are preferred over warfarin for most patients due to their reliability, safety, and freedom from frequent blood tests.
Rate-Controlling Medications
When AF is accepted, controlling the resting and exercise heart rate to comfortable levels reduces symptoms and protects the heart muscle from rate-related weakening.
- Beta-blockers (bisoprolol, carvedilol)
- Rate-limiting calcium channel blockers
- Digoxin (in selected patients)
DC Cardioversion
A brief controlled electrical shock under sedation resets the heart to normal rhythm. Most effective when performed early. Anticoagulation is required for several weeks before and after the procedure.
AF Ablation
A catheter procedure targeting the electrical triggers of AF — typically around the pulmonary veins in the left atrium. Targeted burns (radiofrequency) or freezing (cryo-ablation) isolate the triggers. Most effective for paroxysmal AF in younger, earlier-disease patients.
Related Conditions
Further Reading
Palpitations
AF is the most common cause of sustained palpitations. Understanding what palpitations are and what investigation is needed helps put AF in the wider picture.
Learn about Palpitations → Risk FactorHigh Blood Pressure
Hypertension is the most common cause of AF. Treating blood pressure effectively can prevent AF from developing or reduce its burden once present.
Learn about Hypertension → ProcedurePacemakers
Some patients with AF develop dangerously slow heart rates requiring pacemaker implantation to maintain an adequate heart rate while rate-controlling medications are used.
Learn about Pacemakers →Diagnosed with atrial fibrillation?
Dr Nijjer offers expert AF assessment and management at 68 Harley Street — including stroke risk assessment, rate and rhythm control planning, cardioversion, and referral for ablation where appropriate.
